By Jeffrey Sonsino, O.D., F.A.A.O.
It is well established that good tear exchange under a contact lens can help prevent microbial keratitis, CLARE, and lens-induced corneal edema.1-5 It makes sense from a physiologic perspective. If you have stasis under a lens, byproducts from normal corneal metabolism accumulate in the post-lens tear reservoir. The late Rob Breece (inventor of the Jupiter scleral lens) called the accumulation of debris in the post-lens tear reservoir “The Toxic Swamp” because of its biomicroscopic appearance.
While I love using scleral lenses for a variety of serious ocular conditions, the problem of tear stasis under the lens is concerning. The post-lens tear reservoir in sclerals has been implicated as a resistor to oxygen transmission to the cornea.6 The stasis also seems to be a source of complications ranging from decreased wear time to corneal edema. Patients who remove and reinsert their scleral lenses frequently (4-5 times daily) tend to have better results.7
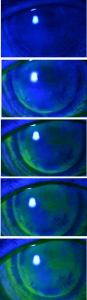
For these reasons, I find myself using hybrid lenses more and more. Hybrid wearers tend to be able to wear their lenses with success from morning to night without having to remove and reinsert. The reason for this is the significant tear exchange observed under the lens. Figure 1 shows times lapse photography (span of 1 minute) of an Ultrahealth lens with no fluorescein placed prior to insertion on a diseased eye (post-PK with significant neovascularization into the graft). The neovascularization was present before fitting with the Ultrahealth lens. You can literally watch fluorescein pumping itself under the lens with each blink.
Figure 1. Time lapse photography (1 minute) of NaFl pumping under an Ultrahealth lens on a post-PK eye with significant existing corneal neovascularization onto the graft.
As evidenced by the above images, Ultrahealth lenses have significant tear exchange in the post-lens tear reservoir in a very short period of time. This may explain the fact that patients wearing Ultrahealth are able to wear their lenses for a full-day’s wear time without having to remove and replace as in sclerals.
Download The Importance of Tear Exchange by Jeffrey Sonsino OD, FAAO
1. Fleiszig SM, Lee EJ, Wu C, Andika RC, Vallas V, Portoles M, Frank DW. Cytotoxic strains of Pseudomonas aeruginosa can damage the intact corneal surface in vitro. CLAO J 1998;24:41–7.
2. McNamara NA, Polse KA, Brand RJ, Graham AD, Chan JS, McKenney CD. Tear mixing under a soft contact lens: effects of lens diameter. Am J Ophthalmol 1999;127:659–65.
3. Creech JL, Chauhan A, Radke CJ. Dispersive mixing in the posterior tear film under a soft contact lens. Ind Eng Chem Res 2001;40:3015–26.
4. Robboy MW, Comstock TL, Kalsow CM. Contact lens-associated corneal infiltrates. Eye Contact Lens 2003;29:146–54.
5. Lin MC, Soliman GN, Lim VA, Giese ML, Wofford LE, Marmo C, Radke C, Polse KA.
Scalloped channels enhance tear mixing under hydrogel contact lenses. Optom Vis
Sci. 2006 Dec;83(12):874-8.
6. Michaud L, van der Worp E, Brazeau D, Warde R, Giasson CJ. Predicting estimates of oxygen transmissibility for scleral lenses. Cont Lens Anterior Eye. 2012 Dec;35(6):266-71.
7. Ortenberg I, Behrman S, Geraisy W, Barequet IS. Wearing time as a measure of success of scleral lenses for patients with irregular astigmatism. Eye Contact Lens. 2013 Nov;39(6):381-4.